Understanding Seizures
Seizures involve sudden, temporary, bursts of electrical activity in the brain that change or disrupt the way messages are sent between brain cells. These electrical bursts can cause involuntary changes in body movement or function, sensation, behavior or awareness.
Every brain has the potential to seize. A person with epilepsy has a lower seizure threshold – this means they are more likely to have seizures than people without epilepsy.
It is important to note the distinction between seizures and epilepsy. A seizure is an event and can be a symptom of other medical problems.
"Not everyone who has a seizure has epilepsy."
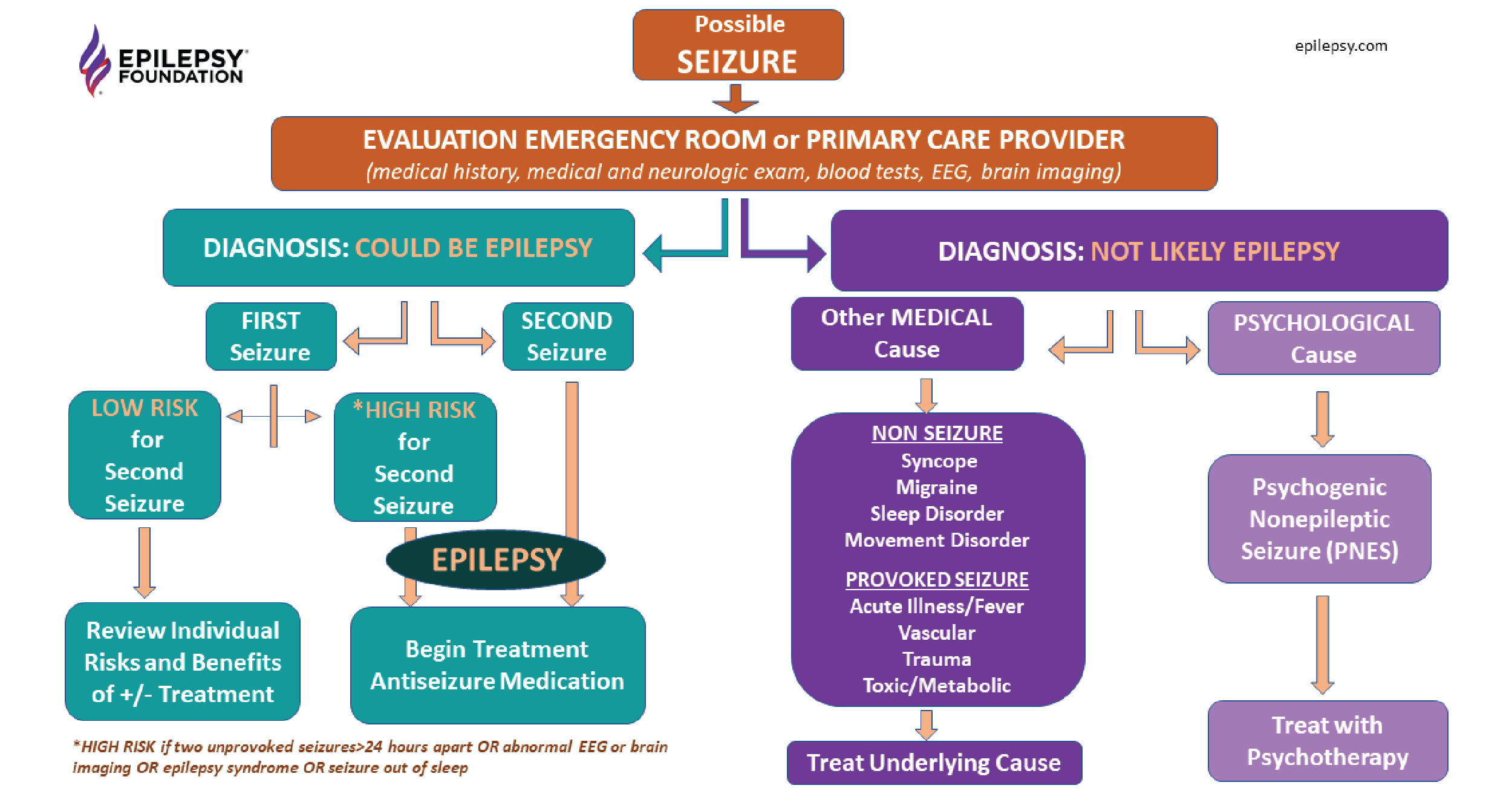
Is this epilepsy?
Epilepsy is a neurological disease. A person with epilepsy is at higher risk for having recurrent (more) seizures. Sometimes people use the words “seizure disorder” to describe epilepsy. Some key facts include
- A diagnosis of epilepsy does not define the cause or the outlook.
- Epilepsy is a spectrum disorder. There are many different types of seizures and types of epilepsy syndromes.
- The impact of epilepsy on a person will vary depending on
- The type, frequency and severity of seizures
- Areas of the brain affected
- Cause of the epilepsy
- How a person responds to treatment
- Underlying brain abnormalities that are present
Treatments available for epilepsy include antiseizure medication, surgery, prescribed dietary therapy, or neurostimulation devices.
What is NOT epilepsy?
What are provoked seizures?
A person can have a seizure from a physical cause. This could be an acute medical illness or trauma that begins before the seizure. It could also be related to a substance or event their body is responding to or withdrawing from. In these cases, seizures are called “provoked.”
The provoking cause has had an effect on the brain that leads to a seizure. These seizures are not diagnosed as epilepsy.
Treatment for provoked seizure should address the underlying cause. Common causes of provoked seizures include
- An acute medical illness (for example, infection)
- A metabolic cause, such as an abnormality in blood sugar
- Fever
- Head injury or brain trauma
- Stroke or transient ischemic attack (TIA)
- Withdrawal from drugs or alcohol
- A reaction to a prescribed or over-the-counter medication
What are nonepileptic events due to other medical problems?
There are also physical or medical events that may mimic or look like seizures. These are not the same as provoked seizures. They are also not due to changes in electrical activity in the brain seen in an epilepsy seizure. Since these are not seizures, they are often called nonepileptic events. Some of these medical conditions include
- Syncope
- Migraine
- Movement disorders
- Sleep disorders
What are psychogenic nonepileptic seizures?
Psychogenic nonepileptic seizures (PNES) also are not caused by abnormal brain electrical activity. PNES may look like epilepsy seizures. They may happen suddenly or start gradually. They may include involuntary changes in behavior, movement, sensation or consciousness that usually last longer than epilepsy seizures. PNES are thought to be the body’s response to physical or emotional distress that the brain is detecting.
- PNES has a psychological origin.
- A person may not be aware of any psychological or distressing factors.
- A person with PNES is not consciously in control their symptoms.
- About 4 out of 5 people with PNES have a history of psychiatric problems, such as depression, anxiety and personality disorders.
- There often is a history of sexual, emotional or physical abuse in people with PNES.
- About half of people with PNES also have a history of post-traumatic stress disorder (PTSD).
- Treament focuses on addressing the underlying cause of the events and helping the person learn new ways of coping.
- Treatment may involve
- Referral to a psychiatrist or therapist
- Medications for anxiety or depression
- Behavioral strategies to manage stress, identify triggers and learning new coping techniques
- Cognitive behavioral therapy (CBT) and other behavioral modification therapies can be an effective treatment for PNES.
- PNES do not respond to antiseizure medications.
Learn More
Resources
Epilepsy Centers
Epilepsy centers provide you with a team of specialists to help you diagnose your epilepsy and explore treatment options.
Epilepsy Medication
Find in-depth information on anti-seizure medications so you know what to ask your doctor.
Epilepsy and Seizures 24/7 Helpline
Call our Epilepsy and Seizures 24/7 Helpline and talk with an epilepsy information specialist or submit a question online.
Tools & Resources
Get information, tips, and more to help you manage your epilepsy.



