Epilepsy Surgery Tests
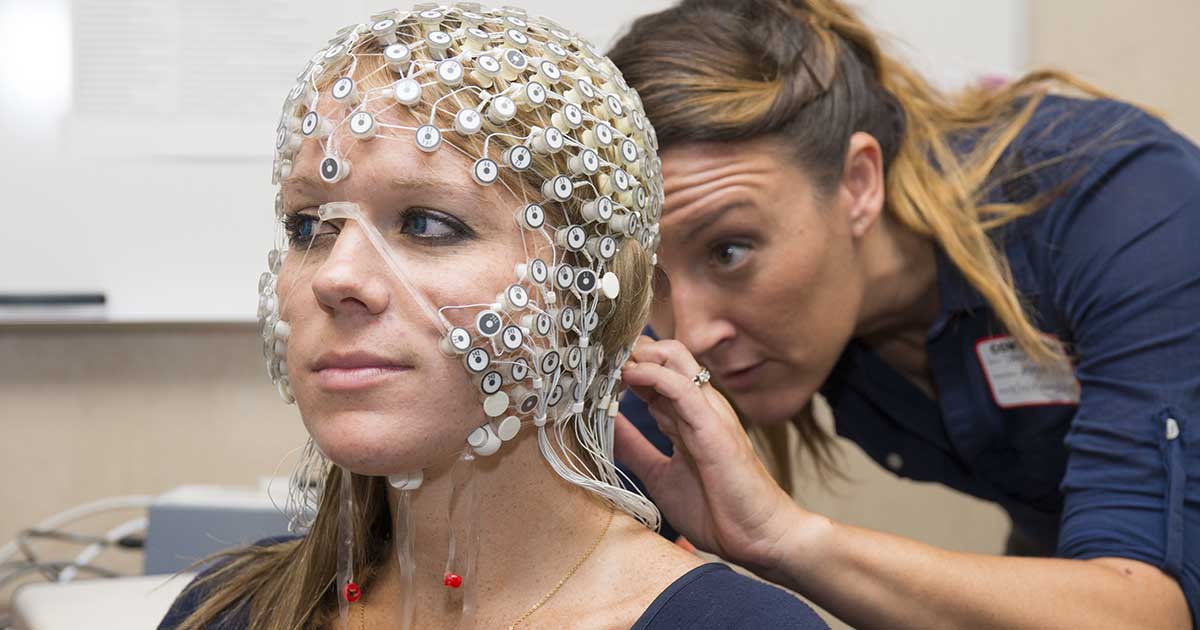
What testing is done during an evaluation for epilepsy surgery?
Testing for epilepsy surgery is aimed at finding out if a person can benefit from surgery to treat their seizures. Testing for epilepsy surgery considers:
- Type of seizures a person has
- Surgical procedure being considered
- Limiting surgical risks and maximizing its benefits
Some tests are common for everyone. Other more specialized tests may be needed for some people. Your epilepsy team will explain why they are recommending the test and how it will help.
A number of tests done before surgery (called a “pre-surgical evaluation”) are done in the outpatient setting. For other tests, a hospital stay will be required.
Outpatient testing helps to:
- Assess a person’s baseline neurologic status
- Make an accurate diagnosis of seizure type
- Assess seizure frequency and impact on a person’s life
- Review past treatment trials
- Determine if a person is drug resistant or if more medication trials and other therapies (such as diet) should be considered
- Determine if routine EEGs (electroencephalographs) are able to show where seizures begin
- Determine if a structural abnormality (lesion) is present on brain imaging (MRI, CT) and if it is the cause of seizures
- Determine if there are problems with memory and thinking
- Evaluate if a person has difficulty with depression or anxiety
- Assess if mood problems are related to seizures or anti-seizure medications
- Assess a person’s day-to-day functional status and quality of life
- Assess a person’s understanding of their epilepsy, their prior treatments, and their readiness to consider surgery
Tell Me More About the Testing
Often people have had several tests done by their outpatient neurologist before they go to an epilepsy center. Your epileptologist (a neurologist who specializes in epilepsy) will determine if this testing needs to be repeated and what new testing should be done.
Evaluation for epilepsy surgery takes place over weeks to months. Although the testing can feel like it is taking a long time, careful evaluation is important. This time also allows you to get to know your epilepsy team, ask questions, and tell them how you feel about possible treatment with surgery.
One way to think about the pre-surgical evaluation is to divide the timeline of testing into phases.
Phase 1: Pre-Surgical Evaluation
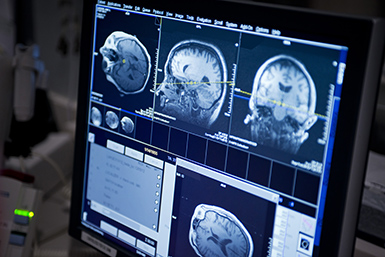
This phase provides a baseline neurological exam, including visual field (vision) testing, and aims to determine the where seizure activity in the brain starts.
- This testing is considered non-invasive testing because no surgery is required.
- It can include outpatient EEG monitoring (person wears an EEG recording device at home) over a number of days.
- In almost all cases, inpatient EEG monitoring and videotaping (called a video EEG) is done to record a person’s typical seizures and compare them with the changes seen on EEG.
- During this testing, usually seizure medication is lowered or stopped so seizures can be recorded and the location where they arise can be found.
- Length of hospital stay can vary from 3 to 10 days and in some cases longer.
- Imaging during this phase may include fMRI, PET, SPECT, or MEG studies.
- Neuropsychology testing assesses language, memory, and cognition.
- A psychiatrist evaluates any mood problems, how this may be related to your epilepsy, and how to treat it.
- A therapist or social worker may help assess how you are coping with epilepsy and the possibility of surgery, as well as what family and friend support you have in your life.
Phase 2: Intracranial Monitoring
After careful review of Phase 1 testing, the epileptologist will talk with the person and their family about findings and possible next steps. For some people, more testing may be needed. This next step is called Phase 2 testing.
Phase 2 testing uses surgically placed electrodes to find out exactly where seizures begin in the brain. Because these tests involve surgery, you can expect to have a pre-operative evaluation that includes:
- Meeting with an anesthesiologist
- A general medical history and physical exam
- A chest X-ray
- An electrocardiogram (ECG)
- Blood and urine tests may also be done
Phase 2 Tests
Intracranial Depth Electrodes (also called Stereo-EEG or SEEG)
Testing with Intracranial depth electrodes is also called Stereo-EEG or SEEG. These electrodes are placed in the brain by a neurosurgeon. They can be put in deeper areas of the brain to find the precise region where seizure activity starts. The electrodes are fine, flexible plastic attached to wires that carry electrical activity from the brain to a recording computer. Imaging studies (CT and MRI) are used to help plan where to place the electrodes. They can also be used to stimulate different areas of the brain to map motor and language functions before surgery. Once the electrodes are in place, they can record seizures for up to 2 to 3 weeks.
Subdural Strip and Subdural Grid Electrodes
These are a series of EEG electrodes mounted on thin plastic that can record electrical activity from the surface of the brain. These electrodes are placed in the operating room. They can be made in a strip or as a square or rectangular grid to cover a larger area of brain surface. Sometimes grid and strip electrodes are used together to cover large areas of the brain when the specific site or lobe of the brain where seizures arise is not clear.
ECoG (Electrocorticography) or iEEG (intracranial Electroencephalography)
ECoG testing involves mapping of brain function that is done in the operating room. This technique uses electrode grids to record activity directly from the surface of the brain (cortex). ECoG/iEEG can help find the specific area of the brain where seizures start and how much to remove during surgery. These electrodes also help find the exact areas responsible for important functions (such as speech, memory, and movement). The spatial resolution of ECoG/iEEG is much higher than scalp EEG recording.
Depending on a person’s individual situation, sometimes this testing is done during phase 2 testing or as a part of the final epilepsy surgery. Your epileptologist and neurosurgeon will decide the best timing for each phase to occur.
Surgical Decision Making
It is important to remember each person’s journey to epilepsy surgery will be different. Your entire epilepsy team will meet and have a “surgical conference” that is dedicated to just your case. They will review all of your testing prior to deciding what epilepsy surgery is best for you.
Examples of how testing decisions may vary include:
- Not all people require Phase 2 or 3 testing.
- Sometimes a brain imaging test (MRI) shows a structural brain lesion (such as a scar from an injury, a tumor, abnormal blood vessels, or an abnormal cluster of neurons) that is in an area of the brain matching their seizure symptoms. In this case, the surgery may be done without extensive EEG monitoring.
- If the neurologic history and exam, imaging studies, and non-invasive EEG do not all point to one area of the brain where seizures start, then Phase 2 monitoring becomes necessary.
The epilepsy team has made a decision. What’s next?
Once your epilepsy team makes their recommendation, you and your loved ones will have time to ask questions and discuss with your doctors and nurses any concerns you may have. It is important to know that in some cases surgery is not possible after a review of all the testing. However, other treatment options may be suggested.
Remember, each member of your epilepsy team is available to support you throughout your journey. Excellent communication with your epilepsy team, comprehensive evaluation and testing, careful surgical planning, and caregiver and family support along the way will all help to make your epilepsy surgery journey a success.
Resources
Epilepsy Centers
Epilepsy centers provide you with a team of specialists to help you diagnose your epilepsy and explore treatment options.
Epilepsy Medication
Find in-depth information on anti-seizure medications so you know what to ask your doctor.
Epilepsy and Seizures 24/7 Helpline
Call our Epilepsy and Seizures 24/7 Helpline and talk with an epilepsy information specialist or submit a question online.
Tools & Resources
Get information, tips, and more to help you manage your epilepsy.



