Relationship Between Sleep Apnea and Seizures
Epilepsy News From: Friday, March 09, 2018
Nancy Foldvary-Schaefer DO, MS, is a professor of medicine at the Cleveland Clinic, where she serves as director of the Sleep Disorders Center and has been on staff at the Epilepsy Center since 1995.
At the American Epilepsy Society annual meeting last December, she presented exciting research on the relationship between seizure control and obstructive sleep apnea (OSA) in people living with epilepsy receiving positive airway pressure (PAP) therapy. Wellness Editor Dr. David Taplinger had a chance to ask her a few questions about this research, and here is what she had to say.
Dr. Foldvary-Schaefer, please describe your study and highlight key findings?
This was a retrospective study of adults living with epilepsy. We divided people with OSA into those receiving PAP and those not receiving it. Between these groups, we looked at who had a 50% reduction in seizure frequency over time.
We found that people treated with PAP were more likely than those who were untreated to have a 50% decrease in seizures (63% vs 14%).
What would you like our readers to know about OSA?
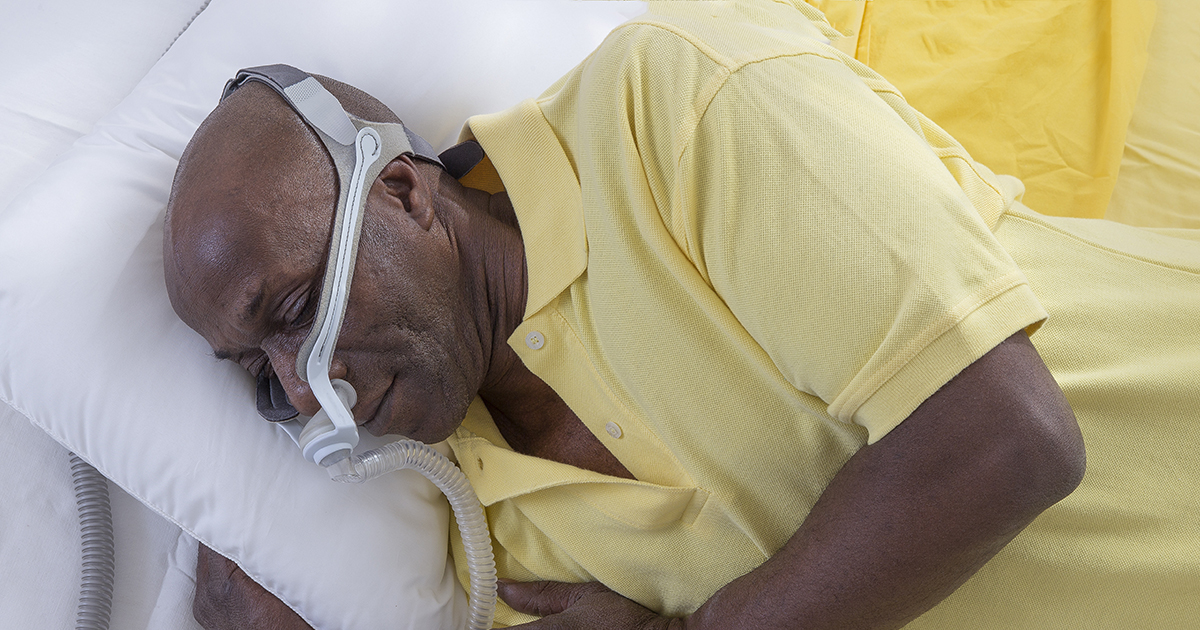
OSA occurs when breathing is interrupted during sleep. OSA is associated with stroke, heart disease, hypertension, diabetes, obesity, and sudden death. It can negatively impact school or work performance.
Sleep disorders are highly common among people living with epilepsy and grossly underdiagnosed. We previously reported a prevalence of OSA in 40% of people living with epilepsy. This does not appear to differ by epilepsy type or degree of seizure control. With treatment for OSA, people often experience improvement in symptoms they previously attributed to seizures or medications.
When should people ask their doctors about OSA?
If they experience poor sleep quality, daytime fatigue or sleepiness, snoring, or breathing issues in sleep, they should talk with their health care provider. It is also important for physicians to ask their patients about these symptoms and to have a low index of suspicion for OSA.
What future directions do you envision for research in this area?
There has never been a prospective, multi-center trial to evaluate the effect of OSA treatment on seizures in people living with epilepsy. Short of that, more work needs to be done to extend these observations to children living with epilepsy, to confirm that beneficial effects extend to everyone living with epilepsy and not just those with refractory epilepsy, and to educate epilepsy caregivers who may not be aware of sleep disorders that impact people living with epilepsy.
Thank you for bringing these exciting findings to light! Before we close, is there anything else you’d like to tell our readers?
Don’t forget about sleep! 30-40% of people living with epilepsy have seizures despite optimal medical therapy. Treating sleep disorders are a novel therapeutic opportunity that should not be missed, especially in people who fail other options.
Learn More
Authored by
David Taplinger MD
Reviewed Date
Friday, March 09, 2018
