From Genes to Epilepsies
Epilepsy News From: Thursday, December 12, 2019
- Some epilepsies have clear genetic connections. They can either run in the family or can be traced to de novo (suddenly occurring) mutations of single genes.
- Others are less clear. Sometimes multiple genes are mutated, and sometimes there are simply no specific genetic mutations.
- Even more frustrating is that the same mutated gene that has little effect in one person can cause severe epilepsy in another.
How do we understand the effects of genes on epilepsy? Is there such a thing as “the gene(s) for epilepsy”?
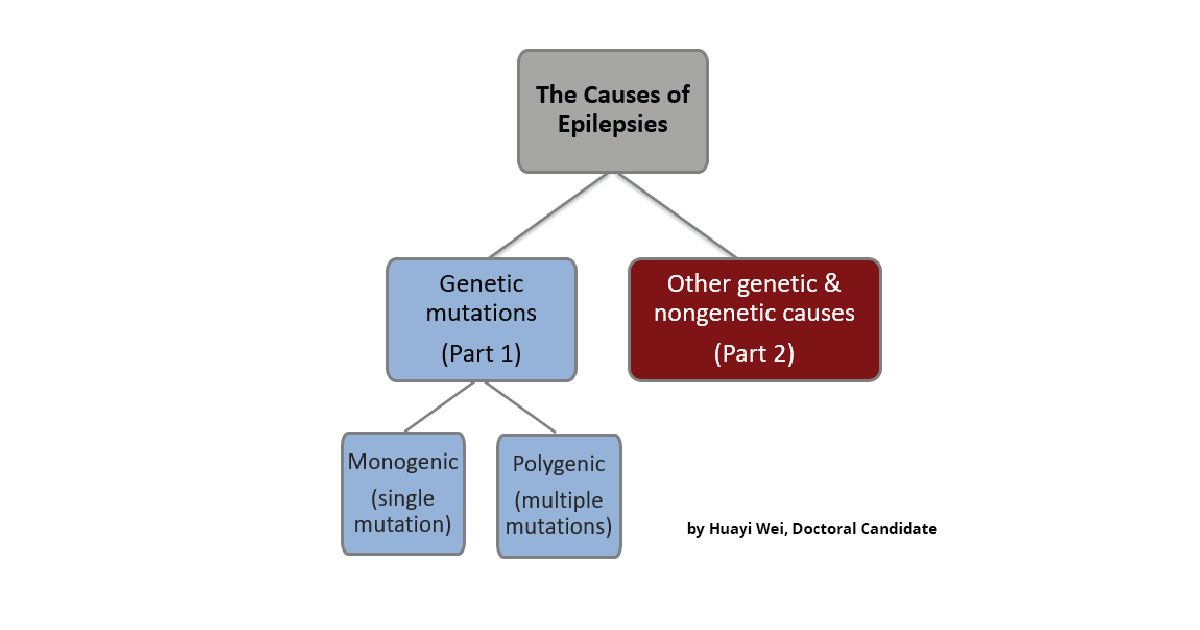
In this two-part article, we will first look into how genetic mutations can lead to either monogenic or polygenic epilepsies. In Part 2, we will discuss other genetic and nongenetic causes of epilepsies.
Genetic Mutations (Part 1)
Monogenic Epilepsies
- Many epilepsies involve genetic mutations. However, some genes have more critical roles than others since the proteins they code for can directly affect brain activities.
- One such gene is KCNQ2. It is the gene for a potassium ion channel. It acts like a tiny gate on the brain cell surface that lets potassium ions escape when the cell is getting too active. As each potassium ion leaves, it carries away a positive electrical charge, discharging the hyperactive brain cells. It is the brain’s version of pressing on the brakes when it’s going too fast. Having a mutated KCNQ2 is as dangerous as having a tampered brake. It can result in unchecked brain activity, which is the hallmark of epilepsies.
- The same critical gene can sometimes contain multiple mutations. But having more places broken doesn’t always mean more severe symptoms. What affects severity is how much the function of the gene is disrupted, or, as an example, how poorly the brake works with KCNQ2 mutations.
- “Monogenic epilepsies” involve the mutation of critical genes like KCNQ2, where a single mutated gene is enough to predict epilepsy. Some examples of KCNQ2 mutation are Dravet Syndrome and Benign Familial Neonatal Convulsions (BFNC). In most of these cases, genetic testing will identify the mutated gene.
- It’s uncommon to see monogenic epilepsies run in families. De novo mutations, mutations that arise spontaneously during cell division are responsible for most monogenic epilepsies.
Polygenic Epilepsies
- “Polygenic epilepsies,” such as Doose Syndrome, involve multiple genetic mutations. Compared to monogenic epilepsies, we understand much less about how polygenic epilepsies start from genetic mutations. To call an epilepsy syndrome polygenic means more than one mutation is associated with the disease.
- Ongoing research proposes that some of these genes may modify the functions of critical genes like KCNQ2, and thus indirectly affect brain activities. A single mutation of these modifiers won’t have a strong effect. But when several mutations combine, their interactions sometimes build up a multiplied consequence.
- Because of the weak effects of an individual genetic mutation, genetic testing often fails to find clear genetic causes for polygenic epilepsies. It becomes more complicated when multiple weak mutations interact with environmental effects and genetic backgrounds to generate epilepsies.
Other Genetic and Non-genetic Causes (Part 2)
Genetic mutations can never fully account for many common epilepsy syndromes, including Genetic Generalized Epilepsy (GGE) (see Terms & Definitions). GGE describes one-third of all epilepsies. In these syndromes, the genetic backgrounds of individuals and environmental factors are thought to play huge roles.
- Our genetic background represents all the genes in our bodies. It varies between families, races and geographical regions. It defines the color of our eyes and the curves in our hair. It also governs how our bodies respond to mutations and environmental stress.
- Some genetic backgrounds appear to be more resilient to mutations. The underlying principles are not known yet. Thanks to the recent progress in genetic sequencing techniques, researchers are gathering an unprecedented amount of genetic information and actively looking at the data for clues.
- One hint is that in some genetic backgrounds the epilepsy-relevant network of genes has a more nuanced (or subtle) architecture. Mutating or removing certain blocks of genes won’t collapse the whole genetic “Jenga” tower. Other genetic backgrounds have their genetic tower balanced differently and would suffer more from the same mutations.
- Similarly, unstable weather conditions and other environmental stress can result in epilepsies in some genetic backgrounds but not others. Our genetic backgrounds control the architectures that handle these factors.
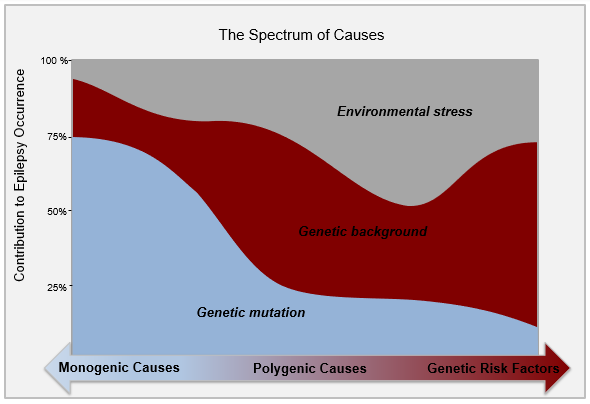
A better way to understand how genes affect epilepsies perhaps requires us to arrange all epilepsy syndromes on a spectrum of causes.
- Monogenic epilepsies are at one extreme, where single gene mutation can contribute 75% and genetic background and environmental effects contribute less.
- At the other extreme, the balance is reversed with genetic mutation contributing only 20% and mutations act more like genetic risk factors.
- Polygenic epilepsies sit in the middle with contributions coming from genetic mutation, genetic background, and environmental factors.
Conclusion
- There is thought to be a genetic component in all epilepsies.
- Some epilepsies are more related to genetic mutations and can be classified into monogenic (single mutation) or polygenic (multiple mutations) epilepsies based on the number of mutated genes.
- Genetic mutation is less significant for the more common epilepsies, which depends largely on genetic backgrounds and environmental factors.
- Epilepsy, just like many neurological diseases, has a spectrum of causes.
References
- Demarest ST, Brooks-Kayal A. From molecules to medicines: the dawn of targeted therapies for genetic epilepsies. Nat Rev Neurol. 2018 Dec;14(12):735–745.
- Gallentine WB, Mikati MA. Genetic Generalized Epilepsies. J Clinical Neurophysiol. 2012 Oct;29(5):408-19.
- Kelley SA, Kossoff EH. Doose syndrome (myoclonic–astatic epilepsy): 40 years of progress. Dev Med Child Neurol. 2010 Nov;52(11):988-93.
- Koeleman BPC. What do genetic studies tell us about the heritable basis of common epilepsy? Polygenic or complex epilepsy? Neurosci Lett. 2018 Feb;667:10-16.
- Motta E, Gołba A, Bal A, Kazibutowska Z, Strzała-Orzeł M. Seizure frequency and bioelectric brain activity in epileptic patients in stable and unstable atmospheric pressure and temperature in different seasons of the year--a preliminary report. Neurol Neurochir Pol. 2011 Nov-Dec;45(6):561-566.
Authored by
Huayi Wei, Doctoral candidate
Reviewed by
Sloka Iyengar PhD
Reviewed Date
Thursday, December 12, 2019
