Childhood Absence Epilepsy
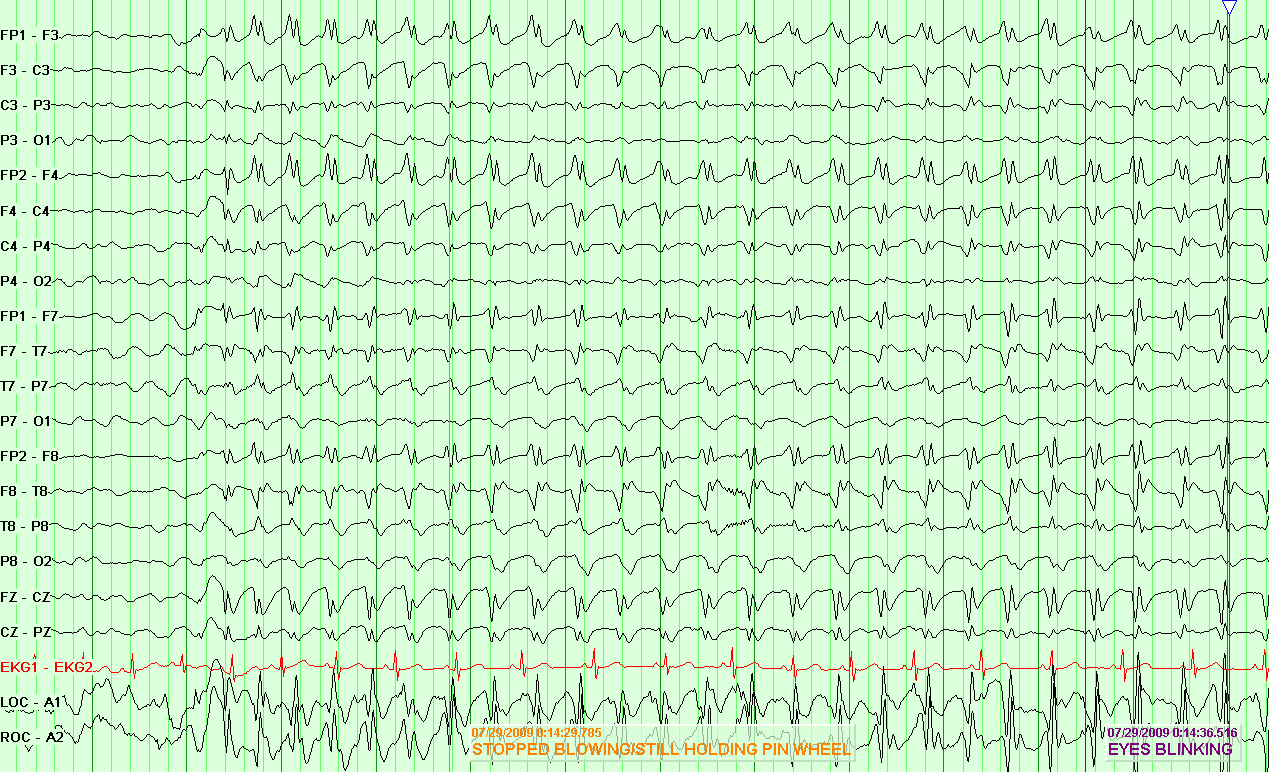
Example of the 3 Hz generalized spike wave
What is childhood absence epilepsy like?
Childhood absence epilepsy (CAE) is an epilepsy syndrome with absence seizures that begin in young children.
- During an absence seizure, the child stares blankly and is not aware or responsive. The child's eyes may roll up briefly or the eyes may blink. Some children have repetitive movements like mouth chewing.
- Each seizure lasts about 10 to 20 seconds and ends abruptly.
- The child resumes normal activity right after the seizure and often doesn’t know that a seizure happened.
- Typically children have multiple absence seizures in a day before medication is started.
- Children usually develop normally, though children with very frequent absence seizures can have learning difficulties. Some children also have attention, concentration, and memory problems.
Learn More:
Find Your Local Epilepsy FoundationWho gets childhood absence epilepsy?
CAE accounts for 1 to 4 out of 50 people with epilepsy (2 to 8%). Absence seizures usually begin between the ages of 4 and 8 years old.
The cause is usually genetic. However, most children with CAE do not have abnormal results on testing for specific epilepsy genes.
- About 1 out of 3 families of children with CAE report a family history of absence seizures or other generalized seizures.
- The brothers and sisters of children with CAE have about a 1 in 10 chance of developing epilepsy.
How is CAE diagnosed?
- A history of the staring spells and any other health and learning problems is the first step in diagnosing CAE. A physical exam looks for other problems that could cause or be associated with the seizures. Children with CAE who have not yet started medicine often will have absence seizures with hyperventilation (deep breathing for 3-5 minutes).
- An EEG (electroencephalogram) is done to look for possible seizure activity. Hyperventilation and photic stimulation (exposure to rapid flashing lights) are often performed during the EEG. The EEG shows generalized spike and wave discharges at 3 Hz (cycles per second).
- CT (computed tomography) and MRI (magnetic resonance imaging) scans of the brain are normal and are not indicated for typical CAE.
- Screening for attention problems is recommended.
How is CAE treated?
- First-line medications (seizure medicines that are most helpful) include ethosuximide, valproic acid and lamotrigine. In most cases, these provide effective seizure control.
- In a recent study, ethosuximide (Zarontin) was shown to be the first drug of choice to treat absence seizures.
- Valproate (Depakote) was equally as effective as ethosuximide, but ethosuximide caused fewer problems with attention than valproate.
- Lamotrigine (Lamictal) was less effective, but certain side effects were less frequent compared to valproate. The side effects generally went away quickly and did not require stopping the drug during the study.
- If absence seizures continue after trying one of these seizure medications, combining these medications may help.
- Other medications have been used to treat absence seizures, like topiramate (Topamax), zonisamide (Zonegran), levetiracetam (Keppra), benzodiazepines (clobazam), stiripentol, and in a few reports amantadine (Symmetrel). These medicines should only be considered if the first-line medications are not working.
- Some children may also benefit from the ketogenic diet if their absences are not controlled by any combination of medicines.
What's the outlook for children with CAE?
- At least 2 out of 3 children with CAE respond to treatment and the seizures disappear by mid-adolescence. In these cases, antiseizure medications can usually be weaned off.
- Problems with attention may continue despite controlling the seizures and are an important part of this epilepsy syndrome.
- Approximately 10-15% of children will develop other seizure types in adolescence, usually generalized tonic-clonic and myoclonic seizures.
Here's a Typical Story
Sonia, a 6-year-old girl, "blanks out" for a few seconds and sometimes stops dancing for 10 seconds during her ballet lessons. Her teacher calls her name, but Sonia doesn't seem to hear her. She usually blinks a few times and her eyes may roll up a bit, but with the short seizures she just stares. Then she is right back where she left off in her dance routine. Some days she has more than 50 of these spells.
What's the difference?
How are childhood absence epilepsy (CAE) and juvenile absence epilepsy (JAE) different?
- When seizures start
- CAE: usually between the ages of 3 and 11 years, most often between 5 and 8 years of age
- JAE: usually between the ages of 9 and 13 years, but could start before age 9
- Frequency of absence seizure
- CAE: multiple, often 10-50, per day
- JAE: often less than daily
- Outlook
- CAE often goes away as the child gets older
- JAE is usually a life-long condition
Learn More:
Contact Our HelplineResources
Epilepsy Centers
Epilepsy centers provide you with a team of specialists to help you diagnose your epilepsy and explore treatment options.
Epilepsy Medication
Find in-depth information on anti-seizure medications so you know what to ask your doctor.
Epilepsy and Seizures 24/7 Helpline
Call our Epilepsy and Seizures 24/7 Helpline and talk with an epilepsy information specialist or submit a question online.
Tools & Resources
Get information, tips, and more to help you manage your epilepsy.



